
Understanding Atrial Fibrillation (AFib) on Apple Watch ECG
Atrial fibrillation, often referred to as AFib, is a common type of irregular heartbeat. It occurs when the heart's upper chambers (the atria) beat out of sync with the lower chambers (the ventricles).
ECG+
4 min read

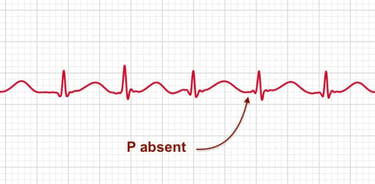
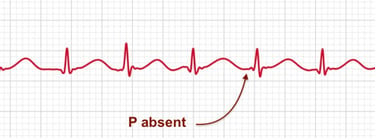
Atrial fibrillation, often referred to as AFib, is a common type of irregular heartbeat. It occurs when the heart's upper chambers (the atria) beat out of sync with the lower chambers (the ventricles). This irregular rhythm can lead to various complications and requires careful management.
On an ECG, atrial fibrillation is characterized by the absence of distinct P waves, which normally represent the orderly contraction of the atria. Instead, the ECG shows rapid, irregular oscillations called fibrillatory waves. The R-R intervals (the time between successive heartbeats) are also irregular, reflecting the chaotic nature of the heartbeat during AFib. This irregularity is one of the key features that helps in diagnosing atrial fibrillation.
How PACs Appear on an Apple Watch ECG
A normal heartbeat on an ECG consists of a P wave, a QRS complex, and a T wave. The P wave represents the electrical activity in the atria, the QRS complex shows the activity in the ventricles, and the T wave represents the recovery of the ventricles after contraction.
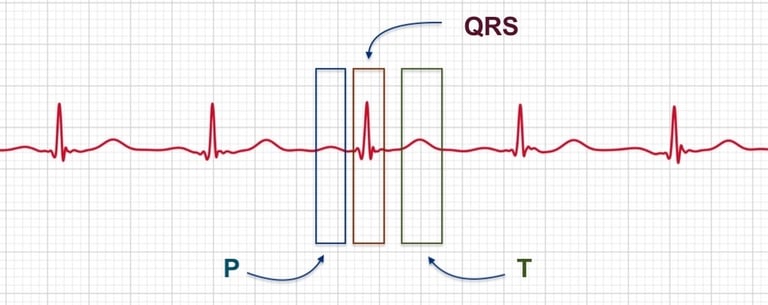
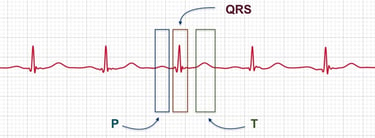
Atrial fibrillation (AFib) occurs when the heart's electrical signals become chaotic, causing the upper chambers (atria) to quiver instead of beating regularly. Normally, a natural pacemaker controls the heart's rhythm, but in AFib, this process is disrupted.
One of the most significant risks associated with AFib is the formation of blood clots in the atria. If a clot dislodges, it can travel to the brain and cause a stroke. AFib also increases the risk of heart failure, especially if it goes untreated. Therefore, early diagnosis and management are crucial to reducing these risks.
Symptoms of Atrial Fibrillation
Managing Atrial Fibrillation
Managing atrial fibrillation (AFib) involves a combination of lifestyle changes, medications, and sometimes medical procedures. The goal is to control the heart's rhythm and rate, reduce symptoms, and prevent complications like stroke.
What Happens During Atrial Fibrillation?
This quivering prevents the atria from effectively pumping blood into the lower chambers (ventricles), leading to blood pooling, which can form clots. If a clot travels to the brain, it can cause a stroke.
The irregular signals also cause the ventricles to beat unevenly, leading to a fast and irregular pulse. This reduces the heart’s efficiency, making you feel tired, dizzy, or short of breath. Over time, AFib can weaken the heart and lead to more serious problems like heart failure.
Risks Associated with AFib
AFib can cause a variety of symptoms, though some people may not notice any at all. Common symptoms include palpitations (a feeling of fluttering or pounding in the chest), fatigue, shortness of breath, dizziness, and chest pain. The severity and frequency of these symptoms can vary widely among individuals.
Rate-control medications: These drugs help slow down the heart rate, ensuring the heart doesn’t beat too quickly. Common medications include beta-blockers, calcium channel blockers, and digoxin.
Rhythm-control medications: These drugs aim to restore and maintain a normal heart rhythm. They are often referred to as antiarrhythmics and may include drugs like amiodarone, sotalol, or flecainide.
Anticoagulants (blood thinners): Since AFib increases the risk of stroke due to blood clots, anticoagulants are often prescribed. These medications, such as warfarin, dabigatran, rivaroxaban, or apixaban, help prevent clot formation by thinning the blood.
Electrical cardioversion: This procedure uses a controlled electric shock to restore a normal heart rhythm. It’s often done under sedation and is usually performed in a hospital setting.
Catheter ablation: During this procedure, a thin, flexible tube (catheter) is inserted into a blood vessel and guided to the heart. The catheter delivers energy to destroy small areas of heart tissue that are causing the irregular signals, helping restore a normal rhythm.
Pacemaker implantation: In cases where the heart rate is too slow after other treatments, a pacemaker may be implanted to help regulate the heart’s rhythm.
Left atrial appendage closure: This is a newer procedure aimed at reducing stroke risk in people who cannot take anticoagulants. It involves sealing off the left atrial appendage, a small sac in the atrium where clots often form in AFib patients.
Ongoing monitoring is crucial in managing AFib. Regular check-ups with a healthcare provider, monitoring your heart rate at home, and keeping track of any symptoms can help ensure that the treatment plan remains effective and any necessary adjustments are made promptly.
Managing AFib is a lifelong process that requires active participation and collaboration between you and your healthcare provider. With the right combination of treatments and lifestyle changes, many people with AFib can lead healthy, active lives.


